On a flight home a few years ago, I was seated next to a VA trauma surgeon completing a second residency, who saw my book title and asked if we could discuss trauma. It is funny the connections we make traveling. We discussed many aspects of trauma, both our own and that of our patients. He described his frustration working with veterans at the VA, because regardless of modality, including surgery, PT, drugs, or therapy, his patients could not open their jaw.
When I explained the freeze response, how in states of high tone arousal core tendon guard can be retained, and the V3 motor lock that accompanies both high arousal and collapse states, he stopped me and said in exasperation, “How do you know this?”
“How much time do you have?”
Three hours later, we were still standing in front of baggage claim, as I taught him how to restore the vagus with his hands.
Polyvagal Theory has given us a framework for understanding the autonomic nervous system in trauma and dysregulation, but it remains largely theoretical: neurological and psychological in its framing, not yet mapped to actual tissue consequences. The jaw that will not open and the neck that will not release are not metaphors. Neither is the enteric nervous system that stops functioning in retained arousal states, the limbic system that goes offline due to GABA flooding, the higher cortical processing that becomes unavailable, or the neuroplasticity that cannot occur in a nervous system still running a survival response. These are mechanical, motor, and neurological events happening in specific tissues at specific anatomical locations.
Until we map the disharmony, we cannot resolve it.
What follows is part of an integrative clinical model that maps this neuroanatomy onto specific anatomical structures and channels, then links it to manual therapy, acupuncture, and Polyvagal-informed trauma work at the tissue level in a framework I call Polyvagal Acupuncture® and Polyvagal Massage™ as its manual therapy counerpart. What requires mapping is not “the parasympathetic system” as a single benign force, but the tone patterns held in tissue, from high tone bracing to collapse, that reflect sympathetic dominance, ventral vagal withdrawal, and deep parasympathetic freeze. The point applications that follow represent only one component of a much larger system. Across neurogenic illness, PTSD, trauma, and Long COVID, the fascial bracing patterns are strikingly consistent in their correspondence to the three primary patterns of autonomic dysregulation, with measurable shifts in tissue tone regardless of diagnosis. These shifts are visible in photographs, legible to both patient and practitioner in real time, and measurable by standard PT, OT, orthopedic, and neurological benchmarks. Most important is the return of the conditions that allow neuroplasticity.
Introducing the Parasympathetic Ganglia
Above T3, the story does not end with the vagus. In the head and upper cervical region, multiple cranial nerves converge within shared anatomical territory. The trigeminal nerve (CN V) shares anatomical and functional overlap with the facial nerve (CN VII), glossopharyngeal nerve (CN IX), accessory nerve (CN XI), and hypoglossal nerve (CN XII), in addition to the vagus (CN X). In high-tone or high-arousal states, especially if primitive reflexes are active, the upper cervical spine can remain spastic and compressed. The parasympathetic ganglia sit within this same field of compression, yet they rarely enter the clinical conversation as named structures.
There are four parasympathetic ganglia in the head. Despite their importance, most acupuncturists never study them directly. Even the major manual therapy traditions that work in the craniofacial field, such as neural manipulation and craniosacral therapy, operate extensively in the same anatomical spaces. JP Barral’s work, for example, engages the pterygopalatine fossa, the infratemporal space, and the orbital structures, yet the parasympathetic ganglia themselves do not stand as the primary organizing map. (Barral, 1999) Classical TCM mapped acupuncture points onto these locations centuries ago, also without naming them. Three independent systems, neuroscience, manual therapy, and Traditional Chinese Medicine, have converged on the same four locations in the head.
In the freeze and fight or flight responses described by PVT, these ganglia are not abstract anatomical structures. They get mechanically compressed and functionally locked when retained. The jaw freezes as V3 motor fibers drive tonic contraction of the muscles of mastication. Speech stops as the Nucleus Ambiguus withdraws its influence on the laryngeal muscles. The tragus cluster locks as the infratemporal fossa compresses around the otic ganglion. Understanding what is actually happening anatomically at each of these sites gives the clinician a precise map for intervention. This is particularly relevant in acute trauma presentations such as those seen in VA and military populations, where autonomic dysregulation is the rule rather than the exception.
The Stomach channel, which runs from the face through the neck and into the thorax, provides a ready-made clinical pathway to either unlock the freeze response or move excess sympathetic charge down and out of the head. The channel’s trajectory passes directly over the otic ganglion at ST 7, the carotid sheath at ST 9, and the thoracic inlet at ST 12, a sequence that corresponds precisely to the anatomical layers of autonomic compression. This document maps that correspondence in detail: first, the four ganglia and their anatomical homes, then their surface projections onto classical TCM points, then the neurophysiology of what happens when these structures lock, and finally, the Stomach channel intervention sequence from clench to drain.
Part 1: The Four Ganglia — Where They Live
- Otic Ganglion
The surface landmark for the otic ganglion is ST-7 (Xiaguan), located in the depression at the lower border of the zygomatic arch, anterior to the condyloid process of the mandible. This is the most deeply situated of the four cranial parasympathetic ganglia and is functionally tied to the parotid gland.
- Bony Space: Located in the infratemporal fossa, immediately inferomedial to the foramen ovale of the sphenoid bone.
- Neural Landmark: It is pinned to the medial surface of the main trunk of the mandibular nerve (V3).
Note: The parasympathetic root of the otic ganglion arrives via CN IX (glossopharyngeal nerve) → lesser petrosal nerve. V3 serves as the mechanical anchor and postganglionic carrier to the parotid via the auriculotemporal nerve, but is not the autonomic input.
Muscular/Vascular Landmarks:
- Medial: Cartilage of the auditory (Eustachian) tube.
- Medial: Tensor veli palatini muscle.
- Anterior: Nerve to the medial pterygoid.
- Posterior: Middle meningeal artery as it ascends toward the foramen spinosum.
Surface Projection: From the lateral aspect, the projection is just above the level of the mandibular notch, deep to the neck of the mandible. This is roughly under the point where the root of the zygomatic arch is palpated, just anterior to the external auditory meatus.
Depth: It sits approximately 45–50 mm deep to the skin, medial to the ramus of the mandible.
The parotid gland occupies a wide surface territory, from just anterior to the ear down to the angle of the mandible. Several TCM points sit within this region: SJ-17 (Yifeng), GB-2 (Tinghui), and SI-19 (Tinggong) all overlie aspects of the gland’s surface. However, these points relate to different structures. SJ-17, in the depression between the mastoid process and the mandible, aligns with the stylomastoid foramen, the exit point of the facial nerve (CN VII). It is not the parasympathetic supply to the parotid.
The parasympathetic supply to the parotid arrives via the auriculotemporal nerve, which carries postganglionic fibers from the otic ganglion. This supply originates deep in the infratemporal fossa — at the level of ST-7, not SJ-17. ST-7 is therefore the functional surface landmark for the otic ganglion’s output, while SJ-17 marks the facial nerve’s exit. Two different systems, operating in adjacent but distinct territories.
- Pterygopalatine (Sphenopalatine) Ganglion
The surface landmark for SI-18 (Quanliao) is in the depression directly infraorbital to the zygomatic bone, aligned vertically with the outer canthus of the eye.
- Bony Landmark: The Pterygopalatine Fossa. This is a narrow, inverted-pyramid-shaped space located between the maxilla (anteriorly) and the pterygoid process of the sphenoid (posteriorly).
- Path to the Ganglion: To reach this space from SI-18, the trajectory passes through the infratemporal space, lateral to the coronoid process of the mandible, entering the pterygomaxillary fissure.
Depth and Placement: The ganglion is located approximately 45–55 mm deep to SI-18. It sits directly inferior to the Maxillary Nerve (V2) as it exits the Foramen Rotundum.
Note: The parasympathetic root arrives via the greater petrosal branch of CN VII (facial nerve), forming the nerve of the pterygoid canal. V2 provides sensory suspension but does not carry the autonomic input.
- Ciliary Ganglion
The surface landmarks involve the medial canthus (UB-1) and the infraorbital ridge (ST-1), providing a pathway into the orbital cavity.
Bony Landmark: The Posterior Orbit, approximately 10 mm anterior to the Optic Canal and the Superior Orbital Fissure.
Path to the Ganglion: The ganglion is situated between the Optic Nerve (CN II) and the Lateral Rectus Muscle. Any projection from the medial or inferior orbital margin must bypass the globe of the eye to reach the retrobulbar space.
Depth and Placement: The ganglion is located approximately 35–40 mm deep from the infraorbital margin. It is anatomically suspended by the branch of the Oculomotor Nerve (CN III) that supplies the inferior oblique muscle.
- Submandibular Ganglion
While often associated with ST-4 (Dicang) or ST-5 (Daying) regions, the ganglion is functionally accessed through the submandibular triangle, medial to the body of the mandible.
- Bony Landmark: The Submandibular Fossa on the medial surface of the mandible, superior to the mylohyoid line.
- Path to the Ganglion: The trajectory is medial to the ramus/body of the mandible and deep to the submandibular gland. It sits on the lateral surface of the Hyoglossus Muscle.
Depth and Placement: The ganglion is located approximately 20–30 mm deep (depending on the angle of approach from the inferior border of the mandible). It is physically suspended from the Lingual Nerve (a branch of V3) by two short communicating branches.
Note: The parasympathetic root of the submandibular ganglion arrives via CN VII (facial nerve) → chorda tympani → lingual nerve. The lingual nerve (a branch of V3) provides mechanical suspension but does not carry the autonomic input.
Part 2: The TCM Surface Map
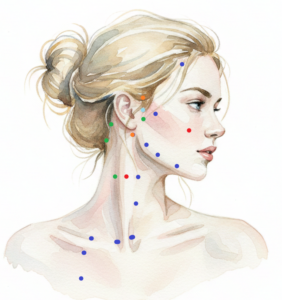 Each of the four ganglia has a direct surface projection onto points that are already part of the classical TCM facial map.
Each of the four ganglia has a direct surface projection onto points that are already part of the classical TCM facial map.
The Pre-Auricular Cluster
The cluster of points directly anterior to the tragus and the mandibular notch corresponds to the anatomical gateways for the deep cranial ganglia. This region is defined by a vertical line of three points positioned between the tragus and the condyloid process of the mandible, with ST-7 (Xiaguan) situated slightly anterior to them.
The Pre-Auricular Cluster (Vertical Line)
These three points are located in the “gate” between the ear and the jaw. From superior to inferior:
- SI-19 (Tinggong): Located in the depression between the middle of the tragus and the mandibular joint. This is the most direct surface projection for the TMJ (Temporomandibular Joint) and the auriculotemporal nerve.
- SJ-21 (Ermen): Located in the depression anterior to the supratragic notch. This aligns with the upper portion of the mandibular condyle.
- GB-2 (Tinghui): Located in the depression anterior to the intertragic notch. Positioned at the lower border of the tragus, directly over the posterior aspect of the mandibular notch.
The Anterior Hub: ST-7 (Xiaguan)
ST-7 is located anterior to the three points listed above. While SI-19/SJ-21/GB-2 sit in the tight space between the tragus and the jawbone, ST-7 sits in the wide depression of the mandibular notch itself.
- Bony Alignment: ST-7 is the specific surface gateway to the infratemporal fossa.
- Deep Structures: Beneath ST-7 lies the otic ganglion and the mandibular nerve (V3) exiting the foramen ovale.
- SJ-17 (Yifeng) Distinction: SJ-17 is located posterior to the ear, in the depression between the mastoid process and the mandible. It aligns with the exit of the facial nerve (CN VII) from the stylomastoid foramen.
Mapping to the Four Parasympathetic Hubs
The “Cluster” anterior to the ear (SJ-21, SI-19, GB-2, and ST-7) serves as the primary clinical access point for the Otic Ganglion and the Trigeminal/Mandibular complex.
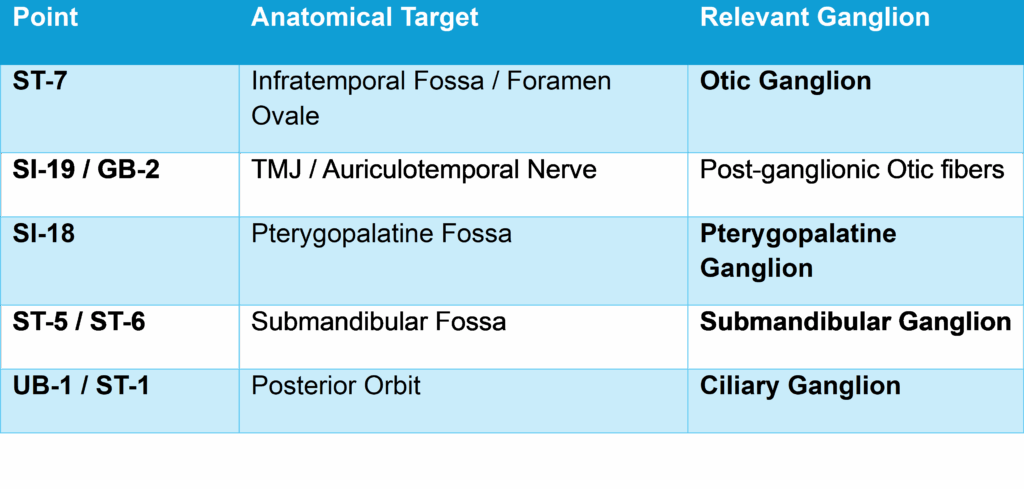

Comparison of the Four Cranial Parasympathetic Hubs
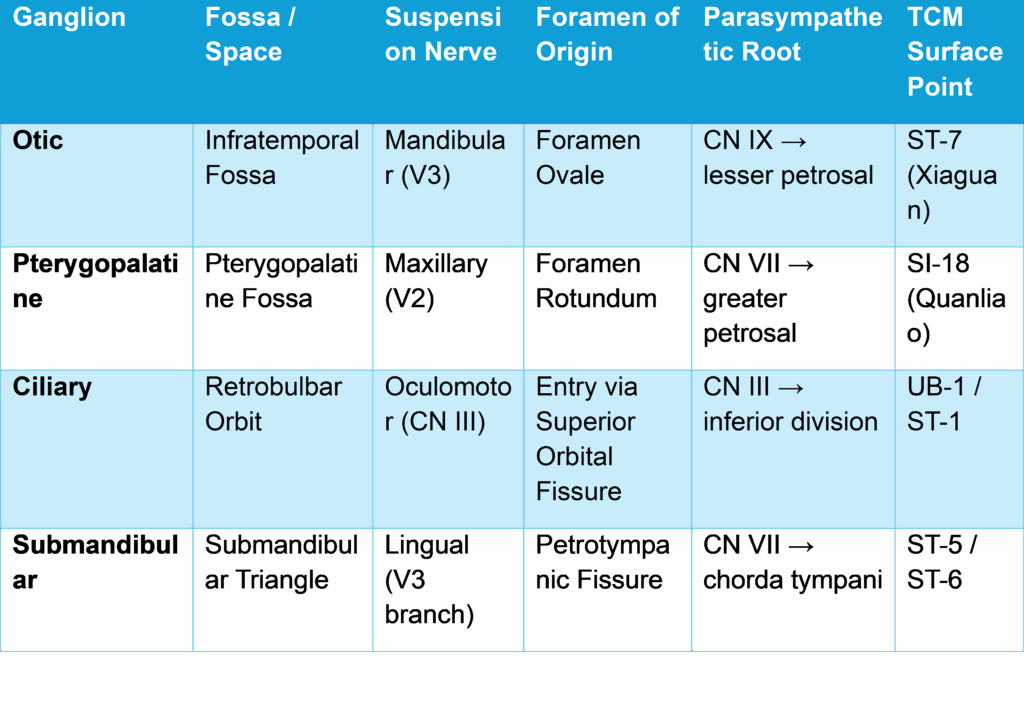
The Otic vs. Trigeminal Distinction
The otic ganglion is physically attached to the medial side of the V3 trunk just below the foramen ovale. Any anatomical projection targeting the otic ganglion via the mandibular notch (ST-7) is simultaneously targeting the most proximal portion of the extracranial trigeminal nerve.

Part 3: What Happens in Freeze and Fight-Flight
Anatomical “Charge” and the Mandibular Notch
The Mandibular Nerve (V3) is the only branch of the Trigeminal nerve carrying motor fibers, specifically to the muscles of mastication (Masseter, Temporalis, Medial and Lateral Pterygoids). In a high-arousal “Fight-Flight” response, these muscles often maintain a state of hypertonicity (clenching), effectively “locking” the mandibular notch.
- V3 and Freeze: In Polyvagal Theory, the transition from high-sympathetic arousal to Dorsal Vagal (freeze) involves a withdrawal of “social engagement” (Ventromedial PANS) and can lead to a metabolic downregulation. While V3 is not literally denervated, its motor output can become “stuck” in a tonic contraction or, conversely, lose the nuanced modulation required for speech and social signaling during a collapse.
- The Otic Ganglion Connection: As the otic ganglion is physically pinned to the medial aspect of the V3 trunk, chronic tension in the infratemporal fossa (at the level of ST-7) creates a mechanical and neurological compression point for the parasympathetic supply to the parotid gland.
The “Silent” Mandible: V3, the Nucleus Ambiguus, and the Neuroanatomy of the Freeze Response
Speech requires the precise coordination of the Trigeminal Nerve (V3) for jaw movement and the Facial Nerve (CN VII) for lip and cheek modulation.
- Mechanical Inhibition: In a high-arousal fight-flight state, the motor fibers of V3 trigger a tonic contraction of the masseter and temporalis muscles (the “clench”). This physiological bracing stabilizes the jaw for impact or exertion but physically prevents the fluid, rhythmic movement required for articulate speech.
- The Laryngeal/Pharyngeal Shift: The Vagus nerve (CN X) provides motor supply to the laryngeal and pharyngeal muscles. During extreme arousal, the Nucleus Ambiguus (the ventral vagal source) reduces its influence, which can lead to a “tight throat” or a loss of vocal prosody (the melodic quality of speech), leaving the voice flat, strained, or entirely absent.
Neuro-Anatomical Summary of Speech Inhibition
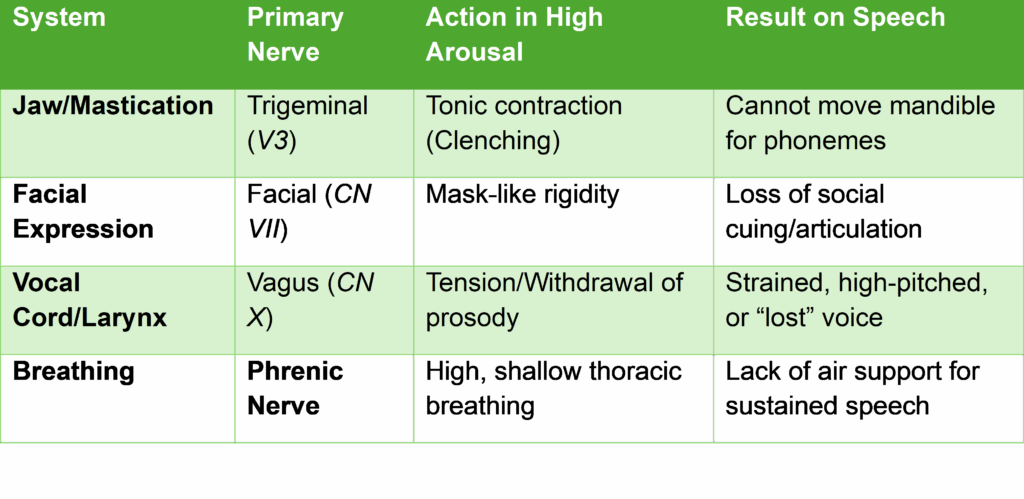
The “Tiger” Logic
When “running from the tiger,” the Nucleus Ambiguus (Social Vagus) and the Trigeminal/Facial social complex are metabolically expensive and unnecessary. Re-establishing the “Social Engagement System” requires the physical unlocking of V3 (at ST-7) and the downward regulation of the sympathetic charge through the cervical “Vagus path” (ST-9 to ST-12).
Part 4: The Stomach Channel — From Clench to Drain (ST-7 to ST-14)
The “Stomach Channel Dump” (ST-7 to ST-12)
Moving “excess charge” down the Stomach channel from the face into the cervical triangles involves transitioning from the Cranial Nerve domain (Head/Face) to the Brachial and Cervical Plexus domain (Neck/Thorax).
- ST-7 as the Valve: Releasing the “clench” at the mandibular notch (ST-7) addresses the V3 motor tension and the deep otic ganglion. This acts as the “opening” of the superior reservoir.
- ST-9 to ST-11 (The Vagus Path): These points sit directly over the Carotid Sheath, which houses the Vagus Nerve (CN X) and the Internal Jugular Vein.
- ST-12 (Quepen): Located in the supraclavicular fossa, this is a critical structural “drain.” Anatomically, this point sits superior to the Cupula of the Lung and the Brachial Plexus, and it is the region where the Thoracic Duct (on the left) empties into the venous system.
The “ST-7 to ST-12” Flow: De-escalating the Charge
Using the Stomach channel to “move the charge down” from the face into the cervical triangles addresses the neurological “clench” at the source.
- ST-7 (Xiaguan): By releasing this point, the tension in the lateral pterygoid and the V3 trunk is addressed. This acts as a signal to the Trigeminal Motor Nucleus in the pons that the “threat” has shifted, potentially allowing for the re-initiation of jaw movement.
- The “Vagus Dump” (ST-9 to ST-12): As the charge moves down the neck, it follows the path of the Carotid Sheath.
- ST-9 (Renying): Sits over the Carotid Sinus, a baroreceptor hub that, when regulated, can help lower heart rate and blood pressure via the carotid sinus baroreflex (baroreceptor reflex) and vagal feedback.
- ST-12 (Quepen): Acting as the “drain,” this point sits at the junction where the head/neck transit meets the thoracic cavity. In a “freeze” state (Dorsal Vagus), the supraclavicular area often becomes rigid. Opening ST-12 encourages the “downward” movement of Qi into the chest and abdomen.
Moving the Charge Down
From a structural integration perspective, “moving charge down” describes the down-regulation of the sympathetic chain (which runs paravertebrally) and the engagement of the Phrenic and Vagus nerves to shift the diaphragm.
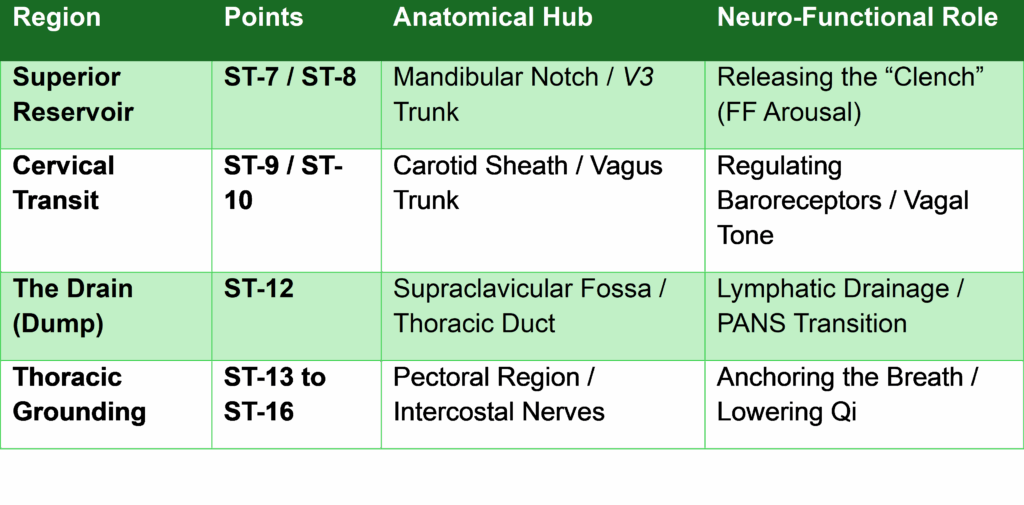

The ST-12 (Quepen) Blockage: The “Drain”
ST-12 is situated in the supraclavicular fossa, directly superior to the cupula (apex) of the lung.
- The Vagal/Phrenic Interface: The Vagus Nerve (CN X) and the Phrenic Nerve (C3–C5) both pass deep to the clavicle in this exact corridor. If the scalene muscles (specifically the anterior and middle scalenes) are hypertonic due to “fight-flight” breathing, they compress the space between the clavicle and the first rib.
- The Thoracic Duct: On the left side, the Thoracic Duct (the main vessel of the lymphatic system) empties into the venous system at the junction of the internal jugular and subclavian veins, directly deep to the ST-12/ST-13 area. A “mess” here physically inhibits the body’s ability to clear metabolic waste from the “vagus dump.”
The ST-13 (Qihu) to ST-14 (Kufang) “Mess”: The Pectoral Guard
As the Stomach channel moves inferiorly over the clavicle into the infraclavicular fossa (ST-13) and the first intercostal space (ST-14), it crosses the Clavipectoral Fascia.
- The Brachial Plexus: The nerves supplying the upper limb emerge through this region. In a protective “collapse” or “freeze” posture, the Pectoralis Minor and the Subclavius muscles shorten, pulling the shoulders forward and “clamping” down on the neurovascular bundle.
- A-P Compression: This “mess” creates an anterior-posterior compression that prevents the “Yang Qi” or high-arousal charge from descending into the lower “Dan Tian” or the abdominal viscera. The charge stays trapped in the neck and head, manifesting as jaw tension (V3 at ST-7) and a “tight throat” (Vagus at ST-9).
Moving the Charge: From “Clench” to “Drain”
Point | Anatomical Obstruction | Impact of Clearing |
ST-12 | Scalene hypertonicity / First rib elevation | Frees the Phrenic nerve; opens the Thoracic Duct for drainage. |
ST-13 | Subclavius tension / Clavicular fixation | Restores mobility to the clavicle; releases pressure on the Subclavian vein. |
ST-14 | Pectoralis minor trigger points | Reopens the chest for deep, diaphragmatic (Ventral Vagal) breathing. |
The Scalene-Serratus Continuum
In structural anatomy models, the Scalenes and the Serratus Anterior are often viewed as a single functional unit or “muscular sling.”
- Serratus Anterior: Originates from the upper eight or nine ribs and wraps around the rib cage to attach to the medial border of the scapula.
- Scalene Muscles: Originate from the transverse processes of the cervical vertebrae (C2–C7) and “wrap” downward to attach to the First and Second Ribs.
Comparison of the “Wrap”
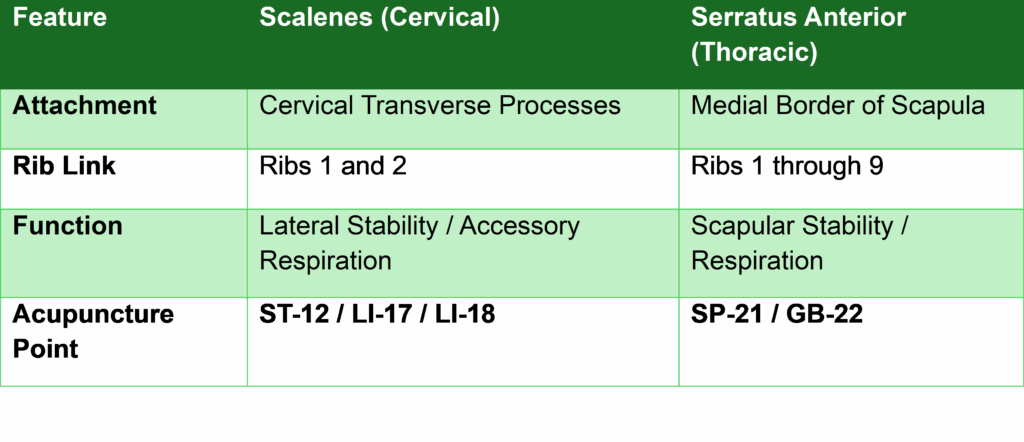
The “Nothin’ Gets Under” Phenomenon
When a client is in an extreme state of arousal or freeze, the First Rib often stays elevated, acting like a closed valve. Until the Anterior Scalene (which attaches to the first rib near ST-12) relaxes, the “charge” cannot move into the thorax. Releasing the V3 clench at ST-7 can sometimes provide the top-down neurological permission for these neck muscles to finally release.
Structural Gates: Top-Down Release Sequence
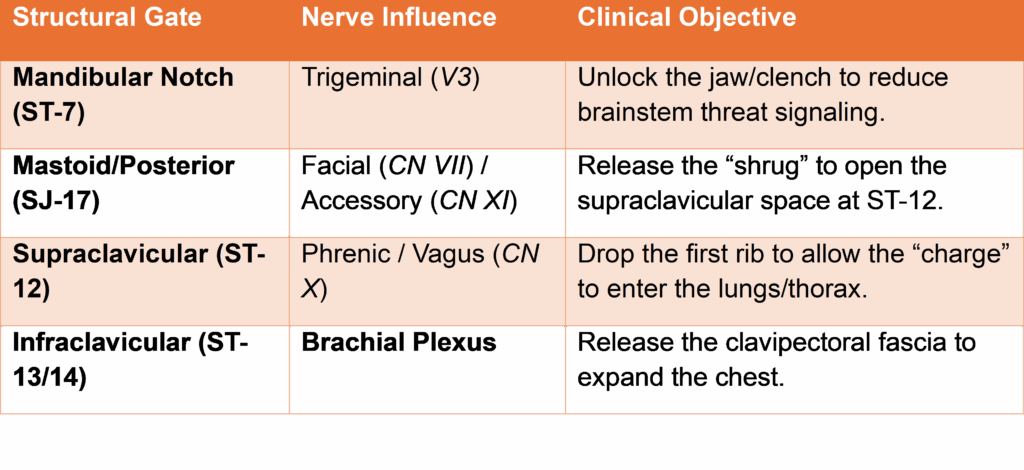
Functional Directionality
- The “Vagus Dump”: Releasing the V3 clench at ST-7 signals the brainstem to reduce threat. The charge is then moved down the carotid sheath (ST-9/10) to the supraclavicular drain (ST-12).
- The Obstruction: Stagnation in the ST-12/13/14 region is caused by an elevated first rib and fibrotic fascia, which prevents charge from entering the thoracic cavity and grounding in the lower body.
In practice, the drainage sequence extends beyond ST-14. Continuing to KD-27 (Shufu), at the first intercostal space medial to the clavicle, opens the T1 level and allows the sympathetic charge to enter the thoracic paravertebral chain and begin its descent. Without this, the charge is released from the above pools at the thoracic inlet rather than continuing downward into the body. This is particularly relevant where cervicothoracic rigidity is present — chronic splenius capitis tension and anterior compression at the cervicothoracic junction create a structural impediment to sympathetic descent. In older patients, and especially in those with a pronounced upper thoracic kyphosis, this bony accumulation of tension at the cervicothoracic junction must be addressed before the full drainage arc can be completed.
The Stomach channel’s trajectory from the face to the supraclavicular fossa is not incidental. It runs directly over the anatomical sequence of PANS ganglia compression, trigeminal motor lock, vagal pathway, and thoracic inlet obstruction that defines the freeze response in the body. Using it intentionally—with an understanding of what lies beneath each point—transforms a classical channel into a precise autonomic intervention.
Part 5: Clinical Considerations
Open the Drain Before the Tap
The Stomach channel sequence from ST-7 to ST-14 is not arbitrary. It follows the anatomical pathway through which excess charge must travel to exit the head and neck. Before any stimulation is applied to the face — whether manual, needle, or electrical — the question must first be asked: Is there patency in the drainage pathway?
If the neck is spastic, the scalenes are locked, and the thoracic inlet at ST-12 to ST-14 is compressed, stimulation above that level has nowhere to go. Working the face while the neck is blocked is not neutral — it risks concentrating charge in a system that has no exit. The drainage must be established before the tap is opened.
Neuroplasticity Has No Hard Ceiling
The clinical consensus that Bell’s palsy and stroke recovery have fixed time windows — six months, six weeks — is based on older models that assumed neuroplasticity had a biological ceiling. Current neuroscience does not support that assumption. Neuroplasticity appears to have no fixed upper limit in a regulated nervous system.
The limiting factor is not time; it is regulation.
Scalp needling and e-stim applied to the head without first clearing the spasticity in the neck creates a sympathetic logjam. The charge has no exit and may drive further contraction through the cervical spine instead of releasing it.”
Case Study: Non-Invasive Neural Regulation in Chronic Bell’s Palsy
[The following case is offered as an illustration of enhanced neuroplasticity and a prompt for further inquiry.]
Patient: Female, 56. Status: 8.5 months post-onset; persistent left-sided hemifacial paralysis. Context: Sustained high allostatic load due to a terminal illness in the family.
Clinical Assessment
- Structural Findings: Rigidity of the occiput, suboccipitals, and lateral myofascial line. Large dowager hump from C5 – T2 (splenius).
- Impingement: Compression at C4 and the internal carotid artery.
- Vascular Verification: Manual pulse comparison. A carotid pulse (ST-9) greater than the radial pulse (local lateral and spiral line impingement).
Treatment Protocol
The intervention consisted of three sessions of Polyvagal Acupuncture® and Polyvagal Massage™, spaced one week apart.
- Session 1: Manual release only. No needles above T3, and no electro-stimulation (E-stim) were utilized. Needles retained distally and on the back. Release lateral line to the clavicular triangle and occipital. Full restoration of motor tone by end of first session.
- Clinical Priority: Establishment of the cervical drainage pathway and decompression of the internal carotid and C4 prior to facial work.
Outcomes
- Session 2: Partial return of hemiplegia. Patient reported normal facial symmetry during periods of ease, with hemiplegia returning during acute stress, demonstrating the direct link between emotional Autonomic Nervous System (ANS) state and physical symptoms.
- Session 3: Full, permanent resolution of low motor tone.
Summary
This document is one component of the Polyvagal Acupuncture® and Polyvagal Massage ™ clinical model. It addresses aspects of treatment for dysautonomia patterns above T3, and introduces the correspondences for the four parasympathetic ganglia of the head and their compression in freeze and fight-flight states.
The Stomach channel sequence from ST-7 to ST-14 is presented as one concrete intervention route within a broader full-body treatment system that includes primitive reflex integration, fascial bracing patterns, and descending autonomic regulation below the thoracic inlet. Neuroplasticity has no fixed ceiling. For those living with demyelinating disease, PTSD, trauma, or stroke, the nervous system retains the capacity to heal when the mechanical and autonomic conditions for that healing are established. The Bell’s palsy case is included as a clinical illustration of neuroplasticity in practice.
References
- Barral, J.-P., & Croibier, A. (1999). Trauma: An osteopathic approach. Eastland Press.
- Barral, J.-P., & Mercier, P. (1988). Visceral manipulation(Rev. ed.). Eastland Press. (Original work published 1983)
- Barral, J.-P. (1989). Visceral manipulation II. Eastland Press.
- Deadman, P. , Al-Khafaji, M. (2007). A Manual of Acupuncture(2nd ed.). Journal of Chinese Medicine Publications.
- Fratkin, J. (n.d.). More Divergent Channel Treatment (Part 4). Jake Fratkin. Retrieved March 13, 2025, from https://drjakefratkin.com/3-level-najom/part-4-more-divergent-channel-treatment/
- Keleman, Stanley. Emotional Anatomy: The Structure of Experience.Berkeley: Center Press, 1985.
- Levine, P. (1997). Waking the Tiger: Healing Trauma.North Atlantic Books.
- Levine, P. A. (2010). In an Unspoken Voice: How the Body Releases Trauma and Restores Goodness.North Atlantic Books.
- Low, R. H. (1984). The Secondary Vessels of Acupuncture: A Detailed Account of Their Energies, Meridians, and Control Points.
- Maciocia, G. (2005). The Foundations of Chinese Medicine: A Comprehensive Text for Acupuncturists and Herbalists(2nd ed.). Churchill Livingstone.
- Masta ova, I. (2005). Integrating Primitive Reflexes for Neurodevelopment.Neurotherapeutics Press.
- Moffitt, J. (2025). The Role of TCM Sinew Channels in Emotional Integration and Vagal Tone Restoration. January 2025.
- Myers, T. W. (2020). Anatomy Trains: Myofascial Meridians for Manual and Movement Therapists.Churchill Livingstone.
- Porges, S. W. (2011). The Polyvagal Theory: Neurophysiological Foundations of Emotions, Attachment, Communication, and Self-Regulation.Norton & Company.
- Pryor, K. (2020). Ten Fingers, Ten Toes, Twenty Things Everyone Needs to Know: Neuroplasticity for Children.Karen Pryor Publications.
- Rosen, J. (2020). Unshakable: Healing the Roots of Trauma.Mindful Living Press.
- Louis Schultz and Rosemary Feitis, The Endless Web: Fascial Anatomy and Physical Reality(Berkeley: North Atlantic Books, 1996).
- Soulié de Morant, G. (1939). L’Acupuncture Chinoise.Éditions Payot.
- Stecco, C. (2015). Functional Atlas of the Human Fascial System.Elsevier Health Sciences.

